If you live in the Pacific Northwest, you know how the shorter days and persistent gray skies can affect your mood. For some people, this goes beyond “winter blues” into something more significant, seasonal affective disorder (SAD). Therapy for seasonal depression offers real, evidence-based ways to address these symptoms, and understanding your options is the first step toward feeling like yourself again.
SAD isn’t something you just have to push through. Effective treatments exist, ranging from specific types of psychotherapy to light therapy, medication, and practical lifestyle adjustments. The key is finding the right combination that works for your unique situation and symptoms. Many people discover that working with a therapist who understands seasonal patterns can make a meaningful difference in how they experience the darker months.
At Healing Connections Counseling, we support adults throughout Portland and Oregon who are navigating depression, including its seasonal form. This article breaks down the therapeutic approaches that actually help with SAD, what the research says, how each option works, and how to figure out which path might be right for you. Whether you’re exploring therapy for the first time or looking for additional strategies, you’ll find practical guidance to help you move forward.
Why seasonal depression needs targeted treatment
Seasonal depression operates differently than other forms of depression because it has specific biological triggers. Light exposure directly affects your circadian rhythm, the internal clock that regulates sleep, mood, and energy levels. When daylight hours shrink during fall and winter, your body produces more melatonin (making you sleepier) and less serotonin (affecting your mood stability). These aren’t just emotional responses to dreary weather, they’re measurable biochemical changes that require targeted interventions.
The biological difference in seasonal depression
Your brain responds to seasonal light changes in predictable ways. The shift in photoperiod (the duration of daylight each day) disrupts the timing of neurotransmitter production, particularly affecting dopamine and serotonin pathways. Research shows that people with SAD often have reduced activity in specific brain regions tied to mood regulation during darker months. This biological component means that willpower alone won’t resolve your symptoms, you need approaches that address the underlying mechanisms.
Standard advice like “just get outside more” or “think positive” doesn’t account for the physiological changes happening in your body when daylight decreases.
The timing of SAD is also important to understand. Your symptoms typically emerge in late fall, peak during winter months, and resolve naturally as spring arrives. This predictable pattern distinguishes SAD from other depressive episodes and points to environmental light as a primary factor, not life stressors or general mental health challenges. Because the trigger is so specific, therapy for seasonal depression includes specialized techniques that directly counter these light-related changes.
Why general coping strategies often fall short
Standard self-care advice doesn’t always work for SAD because it doesn’t address circadian disruption. Taking a walk outside on a cloudy Portland afternoon might provide some benefit, but the light intensity is still far below what your brain needs to regulate melatonin properly. Even sitting near a window indoors typically delivers only about 1,000 lux of light, while your circadian system needs exposure to at least 10,000 lux to shift effectively.
Similarly, general depression treatments may not consider the seasonal component. Antidepressants prescribed without acknowledging the pattern might help somewhat but miss the opportunity to time interventions more effectively. Some people benefit from starting treatment before symptoms typically appear, while others need specific therapies that target light exposure. Targeted approaches recognize your symptoms as cyclical rather than constant, allowing for preventive strategies that match the calendar and your body’s predictable response to seasonal changes.
How therapists treat seasonal depression
Therapists use several evidence-based approaches when working with seasonal depression, with Cognitive Behavioral Therapy adapted for SAD (CBT-SAD) showing particularly strong results. This specialized form of therapy addresses both the behavioral patterns and thought processes that worsen during darker months. You work with your therapist to identify specific triggers, challenge unhelpful thinking patterns, and develop practical strategies that directly counter seasonal symptoms. Research consistently shows that CBT-SAD produces lasting benefits, often reducing symptom recurrence in following winters.
Cognitive behavioral therapy for SAD
CBT-SAD differs from standard depression therapy because it focuses specifically on seasonal triggers and patterns. Your therapist helps you recognize how reduced daylight affects your behavior, such as withdrawing from activities or sleeping more than needed. You learn to challenge thoughts like “I can’t function in winter” and replace them with more balanced perspectives. The therapy also includes behavioral activation, where you deliberately schedule rewarding activities even when motivation drops.

One of the most effective components is learning to anticipate and prepare for seasonal changes before symptoms intensify.
Treatment typically involves identifying activities that boost your mood and energy, then creating structured plans to maintain these behaviors throughout darker months. Your therapist might help you develop a specific schedule for outdoor time, social connections, and meaningful activities that directly counteract seasonal withdrawal patterns.
What happens in therapy sessions
Sessions for therapy for seasonal depression usually occur weekly and last about 50 minutes. You start by tracking your mood patterns and symptoms to establish baseline measurements and identify specific problem areas. Your therapist guides you through exercises that challenge negative thought patterns and helps you practice new behavioral responses. Between sessions, you complete homework assignments that reinforce skills and gradually build sustainable habits. Most people notice meaningful improvements within 6 to 8 weeks, though treatment length varies based on individual needs and symptom severity.
Light therapy and daily habits that help
Light therapy stands as one of the most researched treatments for seasonal depression, with decades of evidence showing significant symptom reduction. You sit near a special light box that emits 10,000 lux (far brighter than typical indoor lighting) for 20 to 30 minutes each morning, usually while eating breakfast or reading. This exposure suppresses melatonin production and signals your brain that daytime has arrived, helping reset your circadian rhythm despite the darkness outside. Combined with consistent daily habits, light therapy creates a foundation that many people find more effective than either approach alone.
Using a light therapy box correctly
Timing and distance matter significantly with light therapy. You need to use the box within the first hour of waking, preferably at the same time each day to reinforce circadian patterns. Position the light at a 45-degree angle above your line of sight, about 16 to 24 inches from your face. You don’t stare directly at the light, instead, you keep your eyes open and let the light reach your peripheral vision while you do other activities. The light needs to enter your eyes to affect brain chemistry, but indirect exposure works perfectly.

Most people notice mood improvements within one to two weeks of consistent daily use.
Start with 15 minutes and gradually increase to 30 minutes if needed. Consistency matters more than duration, so maintaining a regular schedule produces better results than occasional longer sessions. If you experience headaches or eye strain, move the box slightly farther away rather than stopping treatment entirely.
Daily routines that support your circadian rhythm
Beyond light therapy, specific habits strengthen your body’s natural rhythms. Wake at the same time every day, even on weekends, to stabilize your internal clock. Go outside during midday hours when natural light is strongest, even on cloudy days. Dim your lights and screens two hours before bed to allow melatonin production to begin naturally. These habits work alongside therapy for seasonal depression by creating environmental cues that support the biological changes you’re trying to achieve.
Medication and supplements: when to consider
Medication becomes a consideration when light therapy and behavioral strategies don’t provide sufficient relief, or when your symptoms severely disrupt daily functioning. Antidepressants, particularly SSRIs (selective serotonin reuptake inhibitors), show effectiveness for seasonal depression by increasing serotonin availability in your brain. Your doctor might recommend starting medication in early fall, before symptoms typically peak, to prevent the full onset of depression. Some people use medication alongside therapy for seasonal depression rather than as a standalone treatment, creating a comprehensive approach that addresses both biological and behavioral factors.
When antidepressants make sense
Medication typically becomes appropriate when your symptoms include severe changes in appetite or sleep, persistent thoughts of hopelessness, or difficulty completing basic daily tasks. Doctors often prescribe bupropion (Wellbutrin) specifically for SAD because it affects both dopamine and norepinephrine, neurotransmitters closely tied to energy and motivation. Treatment usually starts 4 to 6 weeks before your symptoms historically begin and continues through early spring.
The preventive timing strategy helps many people avoid the full intensity of seasonal symptoms rather than treating them after they develop.
Your response to medication typically takes 2 to 4 weeks, so patience during the initial period matters. Some people benefit from year-round treatment if they experience depression outside winter months, while others taper off medication in spring. Regular check-ins with your prescriber help ensure the dosage remains appropriate and side effects stay manageable.
Vitamin D and other supplements
Vitamin D supplementation addresses a common deficiency that worsens during darker months, though research shows mixed results for mood improvement. Your body produces vitamin D through sun exposure, which drops significantly in Portland winters. Blood tests determine if you need supplementation, typically 1,000 to 2,000 IU daily. Omega-3 fatty acids show some promise for depressive symptoms generally, though evidence specific to SAD remains limited. Talk with your healthcare provider before starting supplements, as they can interact with medications and some people need higher doses than standard recommendations suggest.
When to get help and what to expect
You should consider professional help when seasonal symptoms interfere with your daily responsibilities, relationships, or overall quality of life. Many people wait too long, hoping symptoms will improve on their own, but early intervention typically leads to faster relief and prevents symptoms from intensifying. Therapy for seasonal depression works best when you start treatment before your mood reaches its lowest point, ideally as soon as you notice the familiar pattern beginning. Most therapists understand seasonal patterns well and can help you develop both immediate coping strategies and long-term prevention plans.
Signs it’s time to reach out
Specific symptoms signal that professional support would help. You’re withdrawing from activities you normally enjoy, struggling to maintain work or school performance, or noticing significant changes in sleep or appetite beyond typical winter adjustments. Thoughts about harming yourself or feelings of hopelessness require immediate professional attention. Contact a mental health provider or crisis line right away if you experience these thoughts.
Waiting until symptoms become severe makes treatment more difficult and recovery slower.
Changes in your ability to manage daily tasks also indicate you need support. You’re missing work or canceling plans repeatedly, having trouble concentrating on basic activities, or feeling disconnected from people who matter to you. These patterns suggest your symptoms have moved beyond normal seasonal adjustment into territory where professional guidance becomes necessary.
What your first appointment involves
Your initial therapy session focuses on understanding your specific symptom patterns and history. The therapist asks about when symptoms typically start, how long they last, what you’ve tried before, and how SAD affects your daily life. You discuss your goals for treatment and what improvement would look like for you. Expect the session to last 50 to 60 minutes, with most of the time spent on assessment rather than treatment techniques. Your therapist will likely ask about sleep patterns, energy levels, social connections, and any previous mental health treatment to create a complete picture of your situation.
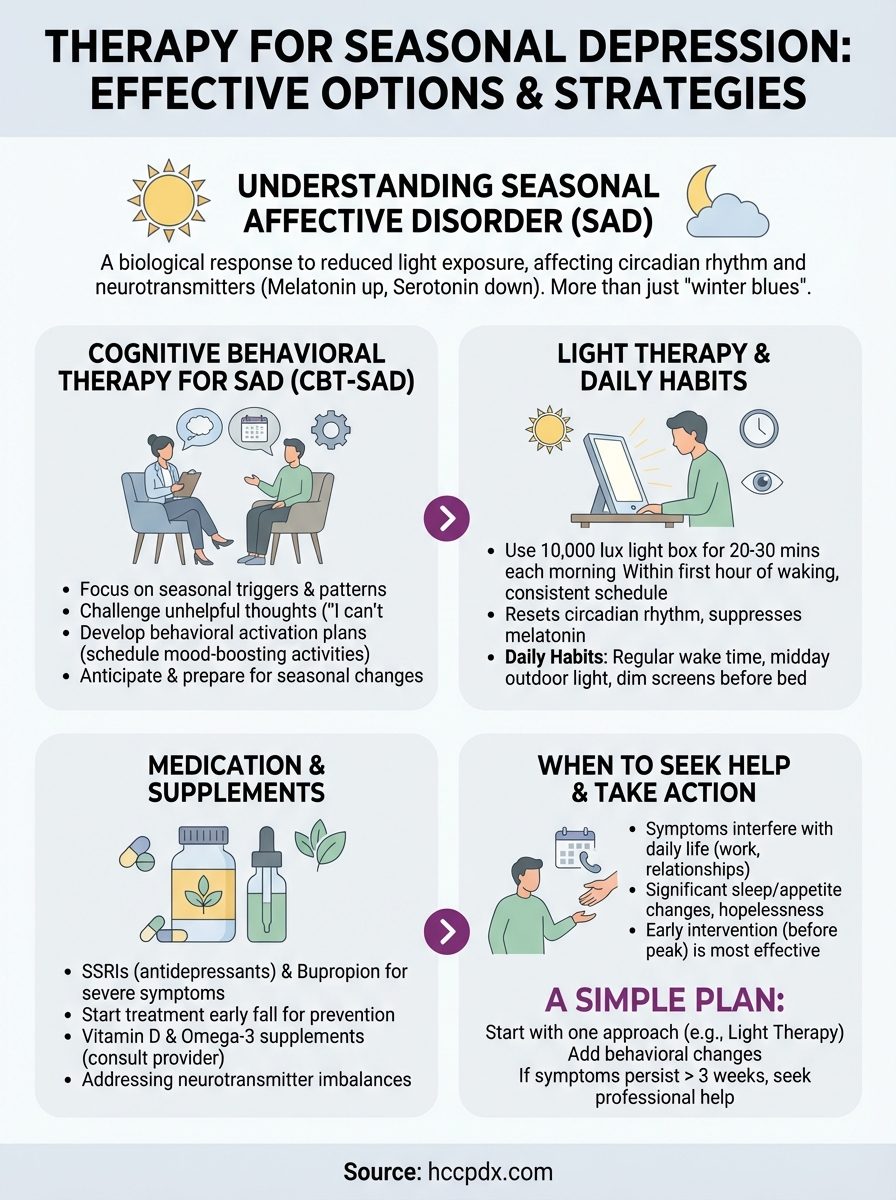
A simple plan for the season ahead
Start by choosing one intervention that matches your current situation. If your symptoms are mild to moderate, begin with a light therapy box used consistently each morning and track your mood for two weeks. Add behavioral changes like maintaining regular wake times and scheduling outdoor activity during midday hours, even when motivation drops.
When symptoms persist beyond three weeks or significantly affect your work or relationships, reach out to a mental health professional. Therapy for seasonal depression works most effectively when you combine approaches rather than relying on a single strategy. Plan to start treatment in early fall next year, before your symptoms typically intensify, to stay ahead of the pattern.
At Healing Connections Counseling, our Portland therapists understand seasonal patterns and provide both in-person and virtual support throughout Oregon. You don’t need to manage this alone, and getting help early makes the darker months significantly more manageable.
